“A Lifeline for Carers”: Ontex supports unpaid carers
Overview
Part of Ontex' ongoing mission is to not only provide excellent quality products, but also to help provide education and training to all of our product users. One very important group are 'Unpaid Carers'. These are the people who are looking after their loved ones on a daily basis having no training and very little support for the work they do. This is why we have partnered with the Grace Cares charity to help provide this information on a local and national level.
Care Club met on Monday 26th January for another supportive session, welcoming unpaid care givers as the club continues to grow. Held in a safe environment, the session gives carers the opportunity to openly discuss their experiences, ask questions and share concerns, while being reassured that they are not alone.
The focus of the session was incontinence care, with practical advice delivered by an experienced incontinence nurse, Paulina Kurek alongside Michelle Garvey from Ontex. Attendees also received additional wellbeing support from Nicola Forsyth who shared guidance on managing stress and overwhelm through life coaching and effective breathwork techniques to help carers regulate and reset during challenging moments.

Care Club is organised by Grace Cares who are dedicated to supporting unpaid caregivers through education, connection and compassionate support. Each session is designed to combine practical guidance with emotional reassurance, while also signposting caregivers to further resources and services that can help them in their caring role. Grace Cares works alongside trusted partners Ontex, to ensure caregivers receive expert, reliable information on topics that are often difficult to talk about.
Paulina from Ontex added: “We’re proud to support Grace Cares’ Care Club in creating open, practical conversations around incontinence, helping people feel informed, supported and less alone.”
For many attendees, the greatest value comes from feeling understood by others in similar situations
One participant shared: “The meetings that I have attended and your team who spoke to me are invaluable to me. Long may it continue. You are providing a lifeline.”

This initiative is part of a global initiative to provide support to unpaid carers, to give them the knowledge to carry on the great work they are doing and to help support their own mental health and wellbeing. You will find a lot of help, support and tips on our Caregivers Connect page which you can view here.
For more information about the training that Ontex offers, please contact [email protected]. If you would like to know more about the great work that Grace Cares does, you can visit their website here: Home - Grace Cares
Keeping Skin Healthy Every Day: Dr. Maria Panourgia’s Practical Tips
“Many patients suffer in silence, not because help doesn’t exist, but because embarrassment stops the conversation.”
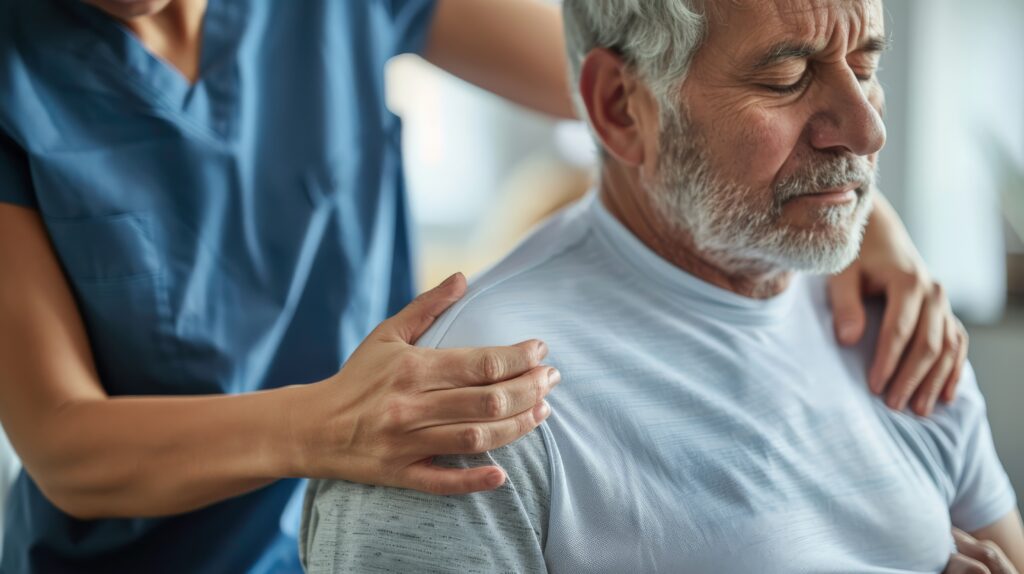
Did you know skin problems are common for people living with incontinence? We asked Dr. Maria Panourgia, a consultant geriatrician, working in Milton Keynes University Hospital, for simple, effective ways to keep skin healthy. Find out what the experts recommend.

Choosing the right incontinence product to protect skin health
Fiona Ecarnot: "What advice do you give patients when choosing an incontinence product to protect the skin?"
Dr. Maria Panourgia: "Many patients already have experience with absorbent products, often from caring for young children. The principles haven’t changed. Comfort is key. The product should not be bulky, should absorb moisture effectively, and should allow freedom of movement.
For people who are mobile, pants products are often the best option. They are easy to use and feel more natural—similar to regular underwear. For people who are bedridden or have limited mobility and rely on caregivers, products that are easy to put on and remove are more appropriate.
Fit is essential. Products should fit snugly without being tight or bulky. Bulky products can create pressure points and increase the risk of skin damage. Equally important is absorption: urine needs to be absorbed and locked inside the pad so moisture does not return to the skin.
Finally, the layer closest to the skin must be skin-friendly—hypoallergenic and breathable. When the skin can breathe, temperature stays lower, and that reduces bacterial growth, which is crucial for preventing infections."
Why using the wrong product can damage the skin?
Fiona Ecarnot: "How can using the wrong product—such as menstrual pads—lead to skin complications?"
Dr. Maria Panourgia: "Menstrual pads and urinary pads are designed for very different purposes. Menstrual products are made to absorb thicker fluids, such as blood, which behaves differently from urine. Urine is much more liquid and requires a different absorption mechanism.
Menstrual pads are not designed to absorb the volume of urine or prevent moisture from returning to the skin. This can lead to leakage, odors, and prolonged skin exposure to moisture. Additionally, urine has a higher pH than the skin. Menstrual pads are not designed to manage this pH imbalance, which can disrupt the skin barrier and lead to irritation and dermatitis.
Urinary pads, on the other hand, are engineered to absorb urine while respecting the skin’s natural pH. The skin is a living system, and it needs protection.
Despite this, around 36% of women still use menstrual pads for urinary incontinence. This is often due to stigma, embarrassment when buying urinary products, or cost concerns. However, in the long term, treating skin infections and dermatitis is far more expensive—physically and financially—than using the correct product from the start."
The role of skin-friendly materials and protective care
Fiona Ecarnot: "Are there benefits to using skin-friendly materials or protective components like zinc?"
Dr. Maria Panourgia: "Absolutely. Protecting the skin is a daily, ongoing task for people with urinary incontinence. Constant moisture can cause maceration, irritation, and incontinence-associated dermatitis. Warm, damp conditions also encourage bacterial and fungal growth, making infections more likely and harder to treat.
Barrier creams—especially those containing zinc oxide—are essential. They create a protective layer that shields the skin from moisture and irritation. Moisturizing creams are also important to keep the skin resilient and healthy.
Prevention is always easier than treatment."
Daily care: what patients and caregivers should do?
Dr. Maria Panourgia: "Pads should be changed as soon as they become wet. This can be challenging, especially for patients with dementia or those in long-term care settings, so caregivers must be particularly attentive.
Urinary pads contain super-absorbent materials that turn liquid into a gel and lock it inside the pad—even under pressure. This technology is effective, but it only works properly if pads are changed regularly.
Good care includes:
- Using the correct urinary product
- Changing pads frequently
- Applying barrier creams
- Moisturizing the skin at every change
Skin should also be checked regularly. Redness, irritation, or areas where a patient repeatedly touches or scratches can be early signs of dermatitis. For people with very sensitive skin, more frequent checks are essential.
Hygiene matters. Clean the area gently with odor-free, hypoallergenic products. Dry the skin by gently patting—never rubbing—to avoid damaging the skin’s protective layer."
Why incontinence-related dermatitis often goes untreated?
Fiona Ecarnot: "Why do you think many people don’t seek treatment for incontinence-related skin problems?
Dr. Maria Panourgia: "It’s a combination of stigma and lack of awareness. Fewer than half of patients report these issues to their doctors. Even though they may speak more openly with healthcare professionals than with others, many still feel uncomfortable admitting the problem.
Urinary incontinence affects a very intimate area—both physically and socially. For people who are otherwise active and independent, it can be especially difficult to talk about."
What healthcare providers can do better?
Dr. Maria Panourgia: "Healthcare professionals need to start the conversation and normalize it. Urinary incontinence is common. It affects both women and men and becomes more frequent with age, childbirth, or pelvic floor damage.
When patients understand that this is a normal, manageable condition, they feel safer asking for help. Early discussions about the right products and skin care can prevent serious complications later—reducing the need for antibiotics or antifungal treatments.
Prevention benefits both patients and the healthcare system."
Improving education for patients and caregivers
Fiona Ecarnot: "How can we improve education and awareness among caregivers?"
Dr. Maria Panourgia: "Around 80% of caregivers are not trained to recognize incontinence-related dermatitis. Unlike pressure ulcers, which are widely documented with visual guides, there is very little practical material available for skin irritation related to incontinence.
We need simple tools: visual guides, short videos, clear instructions. Caregivers should be able to recognize early signs, apply basic treatment like zinc cream, and know when to escalate the issue to a healthcare professional.
Untreated skin irritation can severely limit a person’s life—preventing them from leaving the house, socializing, or even thinking clearly. In vulnerable patients, such as those with dementia, irritation can lead to delirium or serious infections.
Education improves quality of life and reduces healthcare costs."
The bigger picture: quality of life and social reintegration
Fiona Ecarnot: "What do you wish more patients understood about the link between incontinence and skin health?"
Dr. Maria Panourgia: "Many people simply don’t connect the two. Because of stigma, they suffer in silence. Urinary incontinence does not define intelligence, productivity, or value. People can live full, active lives and still experience this condition.
When managed properly—with the right products, skin care, and support—people can continue working, socializing, and living with dignity.
We openly discuss many other health conditions today. Urinary incontinence should be no different. It is a medical condition, and solutions exist."
When preventive skin care should begin
Dr. Maria Panourgia: "Preventive care should begin immediately—ideally before irritation appears. The perineal area is already prone to moisture and limited airflow, even without incontinence.
Once urinary incontinence is present, hygiene and skin protection become even more important. If irritation develops despite proper care, medical review is necessary to rule out infection and start appropriate treatment.
Prevention is always the first step. Treatment comes later—when prevention has failed."
Meet our new iD Sensitive product range
Powerful protection, soft on skin
Designed for skin that helps to prevent irritation.

Case Study - Transforming Continence Care with UHDB (University Hospitals of Derby and Burton
Overview
Following a review of continence product usage and expenditure, University Hospitals of Derby and Burton (UHDB) – Royal Derby Hospital identified unusually high usage of certain continence products. The aim was to establish a standardised product formulary across all five hospital sites, evaluate usage patterns, and understand variation in clinical practice.
Led by Anita Counsell, Lead Urology Clinical Nurse Specialist (CNS), and supported by Sheryl Stone (Account Manager at Ontex) and Naomi Gill,(Nurse Advisor at Ontex), the project set out to improve staff awareness, ensure appropriate product use, and reduce variation across wards. This was the Trust’s first unified approach to continence product provision.
“The key to the success of this project was that we all worked together so well. We were on the same page, focused on improving training, education, and support to create a uniform formulary. Regular meetings made the process a smooth transition.” – Sheryl Stone, Ontex Nurse Advisor
Data Analysis and Product Evaluation
The Urology CNS and Procurement teams conducted a comprehensive review of continence pad usage across all sites, mapping product volume, type, and brand. This detailed analysis revealed inconsistent product use, disproportionate consumption, and instances of inappropriate selection.
All suppliers on the NHS framework were assessed. Following clinical and commercial evaluation—including a tabletop assessment of pad quality and cost-effectiveness—Ontex was awarded the contract Trust-wide, retaining their existing position at Royal Derby Hospital and expanding to all other sites.
The procurement team worked with the Urology team to ensure that the selected supplier could provide not only the right product but also the implementation support and training necessary to embed change across a large, multi-site organisation.

Implementing Change
The project’s success hinged on three factors: accurate data, clear communication, and effective training.
Sheryl and Naomi worked closely with the Urology and Procurement teams to plan a Trust-wide rollout. Sheryl developed a digital support pack, ensuring ward teams received educational tools to complement physical training sessions.
The introduction of a restricted formulary allowed UHDB to standardise products, reduce waste, and streamline procurement. For example, high-absorbency pads, which were often used unnecessarily as a time-saving measure, were removed from general ordering, improving both cost efficiency and clinical practice.
Ontex played a critical role in supporting the transition. Their ward-based education, tailored to each department’s needs, reinforced correct fitting, product selection, and patient assessment. Their physical presence during rollout helped ensure the changes were understood and accepted.
“Challenging established practices is never easy,” noted Anita. “Some wards had routines based on habit rather than assessment. We needed to back the changes with training and clear guidance on appropriate clinical exceptions.”
Initial resistance—particularly to less absorbent pads—was addressed through practical demonstrations and staff support. Ontex’s involvement in training helped build confidence and flag areas requiring further attention from the Urology CNS team.
Monthly implementation reviews were held in the first year, followed by quarterly check-ins. Compliance data from Procurement and regular updates from Ontex Nurse Advisors ensured sustained progress and prompt resolution of any issues.
Impact and Outcomes
One year post-implementation, UHDB reported:
- £40,000 cost saving through reduced waste and streamlined product use
- Improved patient continence care, with more appropriate pad selection and change routines
- Increased staff knowledge, supported by
regular training and digital resources - Alignment between acute and community teams, enabling smoother transitions of care
“While cost reduction wasn’t our primary goal, this project has clearly improved patient outcomes, staff practice, and financial efficiency. The collaboration between the Trust and Ontex has been a major success.”
If you would like to receive continence training from Ontex please contact us at [email protected]
For more information on Ontex products, please visit https://ontex.com
Case Study - Creating Care Pathways for Paediatric Continence in Remote Communities
Establishing a Children’s Continence Advisory Service in Orkney: A Collaborative Journey
Orkney School Health Team had observed a steady increase in the number of children experiencing continence issues across the region. Families were seeking advice, treatment, and access to suitable products — yet there was no dedicated pathway in place to support them. Historically, paediatric patients had been referred into the adult continence service, where products were often issued without the child being assessed in person. While this approach may have met some immediate needs, it did not account for the complexity of continence care in children — where developmental, behavioural, and medical factors often require tailored support.
The limitations of this system became increasingly evident to the School Health Team, who recognised the urgent need to develop a dedicated children’s continence advisory service. However, for the small team based at The Balfour Hospital — in one of the UK’s most remote island communities — this presented a significant challenge. They lacked a clear model to follow, had limited experience in paediatric continence care, and were operating within tight financial and logistical constraints.
Who was involved?
Thisbe Sinclair - School Nurse
Hannah Leslie - Trainee School Nurse
Alison Reid - Staff Nurse
Marie McGregor - Nurse Advisor Ontex
Sunni Liston - Nurse (ERIC)
Taking the First Steps
The initiative was spearheaded by three committed nurses: Thisbe Sinclair (School Nurse), Hannah Leslie (Trainee School Nurse), and Alison Reid (Staff Nurse). Driven by a shared determination to improve care for local children and families, they began exploring options for setting up a new service. However, with no clear starting point and limited local resources, they soon realised they would need external support.
After conducting initial research, the team reached out to Ontex, a continence care supplier with experience in supporting healthcare services across the UK. Their first point of contact was Marie McGregor, Ontex Nurse Advisor, who quickly became an important partner in the project. Marie worked closely with the team to understand their needs, challenges, and goals, and began arranging regular support meetings to guide them through the process of building the service from the ground up.
Marie also connected the School Health Team with Sunni Liston, a specialist nurse affiliated with ERIC, the national children’s bowel and bladder charity. Sunni brought essential insight and clinical experience, helping the team understand best practices for setting up a paediatric continence service in a remote context. Together, Marie and Sunni helped the School Health Team select a product formulary appropriate for children, provided training on how to use and assess the products, and shared guidance on referral pathways, care planning, and ongoing review processes.
“It was all very challenging in the beginning — we didn’t know where to start. But with Sunni and Marie’s support, we managed to identify the best products for our children and created a formulary that works for all of us. It’s been great to see what we’ve achieved in such a short time.”
— Thisbe Sinclair, School Nurse
Navigating the Challenges of Remote Healthcare
Several of the barriers faced by the team were unique to Orkney’s geography and infrastructure. As a rural and remote community, Orkney does not benefit from the dense healthcare networks found on the mainland. Patients and families may need to travel significant distances — including by ferry or air — to attend appointments. This makes regular face-to-face assessments particularly difficult, especially for children and families already under strain.
The team adopted a pragmatic approach: the initial assessment would be conducted in person to ensure the child received appropriate, well-fitted products. Following this, reviews and adjustments could often be managed via telephone, with reassessments arranged as needed. This hybrid approach helped balance quality care with practical realities, ensuring that children received support without overburdening families or staff.

“We’ve learned so much about how to run a continence advisory service, and how we can best support children, young people and their families through this process. It’s been a steep learning curve, and one that we will continue gaining knowledge in!”
— Alison Reid, Staff Nurse, School Health
Building Confidence and Capacity
For the School Health Team, the experience of building a service from scratch has been both challenging and empowering. The partnership with Ontex and ERIC not only brought expert knowledge and training, but also gave the team the confidence to make clinical decisions, communicate effectively with families, and advocate for the needs of children in their care.
Impact on Families and the Wider Community
Though still in its early stages, the new children’s continence advisory service has already made a meaningful difference to local families. Children are now receiving assessments appropriate to their age and needs, with care plans tailored to support their independence, dignity, and long-term development.
The success of this project has also opened the door to wider conversations about children’s health in Orkney, and there are hopes that the service can be expanded further to include more education and early intervention support for schools and families.
“It’s been very helpful to know that Ontex have been there to support us on this journey. Setting up the continence service was something we’d been wanting to do for a long time — we just didn’t have the support or know-how to make it happen.”
— Hannah Leslie, Trainee School Nurse
Ongoing Support and Future Plans
Marie McGregor and the Ontex team continue to provide ongoing support to Orkney School Health Team, with regular check-ins and updates on product developments, best practices, and clinical guidelines. ERIC also remains a key partner, offering expert advice and access to a broader network of paediatric continence specialists.

The Orkney team now looks ahead to strengthening the service further, exploring ways to embed continence education into school nursing, community outreach, and partnership work with the Health Visiting team. They hope to share their experience with other rural teams, showing that — with the right support and determination — even small, remote services can deliver high-quality, child-centred care.
If you would like to receive continence training from Ontex please contact us at [email protected]
For more information on Ontex products, please visit https://ontex.com
New White Paper Exposes Hidden Crisis Facing Unpaid Caregivers in the UK
Grace Cares, in collaboration with Ontex Global, has released a powerful new white paper highlighting the urgent need to support the UK’s millions of Unpaid Caregivers. This group is too often overlooked in policy, services, and public understanding.
Titled “Caring by Love, not by Pay: Stories and Solutions from Unpaid Caregivers”, the report is based on a national survey and in-person consultations with over 75 Unpaid Caregivers. It brings their lived experiences into sharp focus, revealing a widespread lack of recognition, poor access to support, and serious impacts on emotional and mental wellbeing

According to Carers UK, there are around 5.7 million Unpaid Caregivers in the UK, providing care worth an estimated £132 billion per year – equivalent to a second NHS. Yet the white paper reveals:
- Many do not initially identify as an Unpaid Caregiver, meaning they miss vital help
- 54% of respondents feel the Unpaid Caregiver role is under-recognised
- 76% are unsure how to access support that already exists
- Over 50% reported emotional and psychological distress from their caregiving role

In response, Grace Cares and Ontex Global are co-developing a programme of local and national resources, drop-in sessions, and peer support initiatives, built directly from what Unpaid Caregivers said they need.
“At Ontex, we are proud to sponsor and support this vital work. Unpaid Caregivers deserve practical solutions, better recognition, and real-world support – not more barriers,” said Emily Vernon, UK Country Manager, Ontex Global.
Recommendations in the report include:
- Better national and local recognition of the Unpaid Caregiver role
- Improved signposting and awareness of existing services
- Access to emotional and psychological support, including counselling and peer networks
- Funding for respite care and training for complex caregiving tasks
- A unified terminology and clearer pathway to identify as an Unpaid Caregiver
What’s next?
Grace Cares is inviting local authorities, health and care leaders, and community partners to act on these findings. Together with Ontex, they aim to build a national movement that ensures every Unpaid Caregiver has access to the support they deserve





